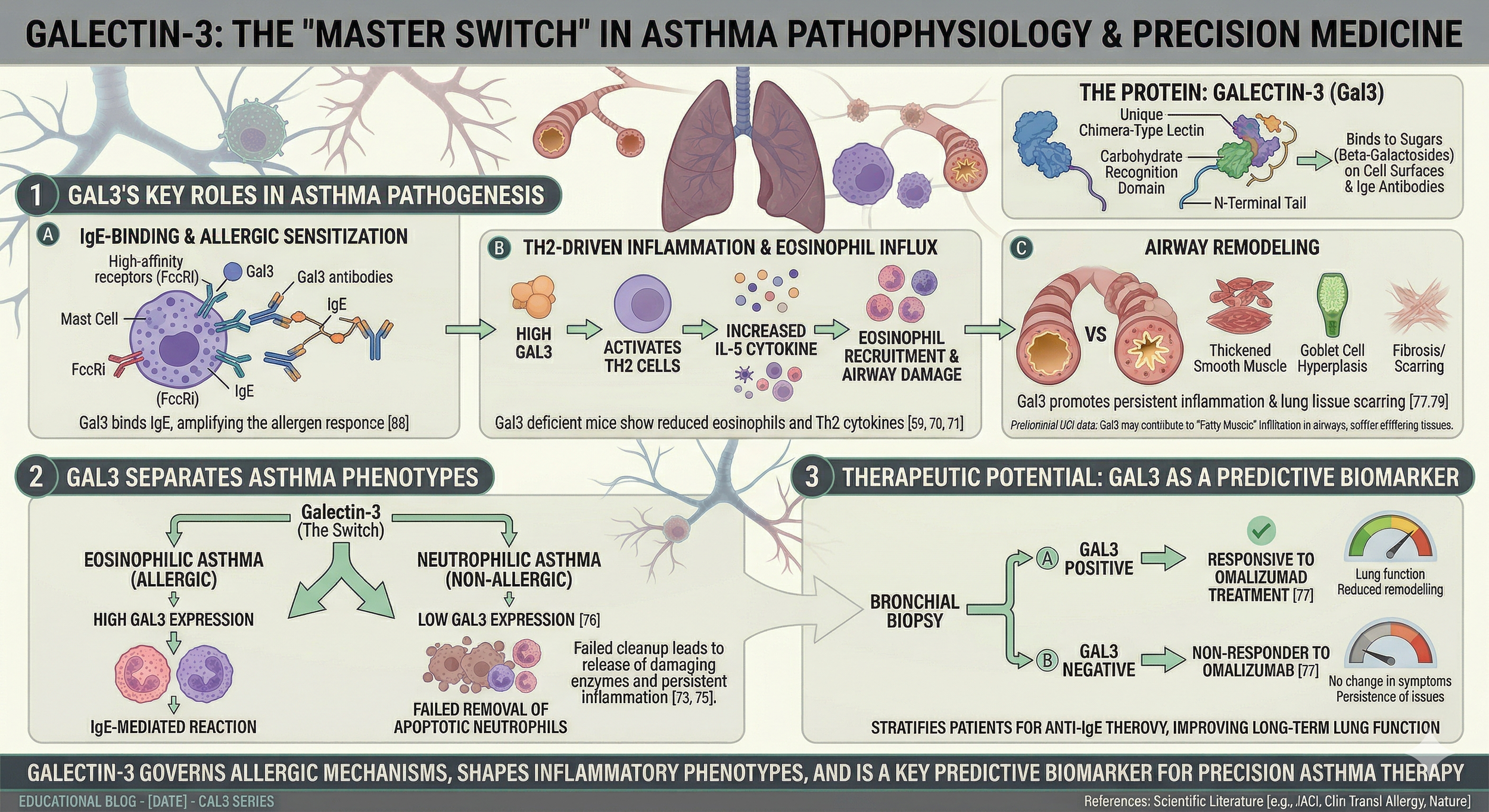
The Airway Architect: How Galectin-3 Shapes Asthma Phenotypes
Asthma
It is a complex, heterogeneous condition characterized by chronic airway inflammation, reversible obstruction, and airway hyperresponsiveness (AHR). For five decades, IgE antibodies have been the undisputed villains in triggering allergic responses.
However, emerging research reveals that IgE does not act alone. It works within a complex protein network, and Galectin-3 has received increasing interest as a master player in this network, acting as an IgE-binding protein that governs inflammation, cell activation, and lung remodeling.
1. The Gal3 and IgE Connection: More Than Just a Binding Partner
Gal3 was initially identified as an IgE-binding protein. While it interacts with high- and low-affinity IgE receptors (FcεRI and FcεRII/CD23), its role goes deeper than simple binding.
Regulator of Infiltration: Gal3 acts as a regulator of the inflammation, activation, and clearance of infiltrating cells in the airways.
Location Matters: Galectins can exert either pro- or anti-inflammatory outcomes depending on their location (intracellular vs. extracellular) and whether they are produced endogenously or delivered exogenously.
2. Gal3: The Switch Between Asthma Phenotypes
Asthma is classified by the dominant inflammatory cell type (phenotype). Gal3 plays a distinct role in separating these types:
A. The Neutrophilic Battle (Non-Eosinophilic Asthma)
In neutrophilic asthma, inflammation persists because apoptotic (dying) neutrophils are not removed efficiently. Gal3 is vital for this "cleanup" process.
The Mechanism: Gal3 normally increases the uptake of apoptotic neutrophils.
The Failure: If Gal3 is dysfunctional, apoptotic neutrophils build up, releasing damaging enzymes and oxidants. This promotes the persistence of inflammation.
The Biomarker: In humans, significantly reduced levels of Gal3 are detected in the sputum of neutrophilic asthma compared to eosinophilic asthma.
B. The Eosinophilic & Th2 Drive (Allergic Asthma)
Gal3 also influences the Type-2 Helper T lymphocyte (Th2) response, which drives allergic inflammation.
Gal3 Deficiency: Studies in Gal3-null mice show reduced airway hyperresponsiveness (AHR), less eosinophil infiltration, and a reduction of Th2 cytokines (like IL-5).
Contradictory Signals: Interestingly, some studies (in Brown-Norway rats) show that introducing the Gal3 gene impaired certain Th2 effects and down-regulated IL-5, suggesting its role is highly context-dependent in chronic vs. acute models.
3. Precision Medicine: Gal3 Predicts Omalizumab Response
The most ground-breaking discovery for patients with severe asthma is the use of Gal3 as a predictive biomarker for stratifying patients for therapy.
The Therapy: Omalizumab is a monoclonal anti-IgE antibody used for severe asthma.
The Challenge: Not all severe asthma patients respond to Omalizumab.
The Gal3 Solution: Analysis of bronchial biopsy specimens before treatment can predict success:
Gal3-Positive Patients: Were responsive to Omalizumab treatment, showing long-term improvements in pulmonary function.
Gal3-Negative Patients: Were non-responders to Omalizumab.
This breakthrough positions Gal3 alongside established biomarkers (like FeNO, eosinophil counts, and periostin) to help doctors determine the best, most effective treatment for individual patients.
Scientific Foundations: The Evidence for Galectin-3 and Asthma



